Blood Cancer Treatment
Your health, our priority – We offer you the finest treatment with personalized care that goes beyond treatment. Reach out to us today.
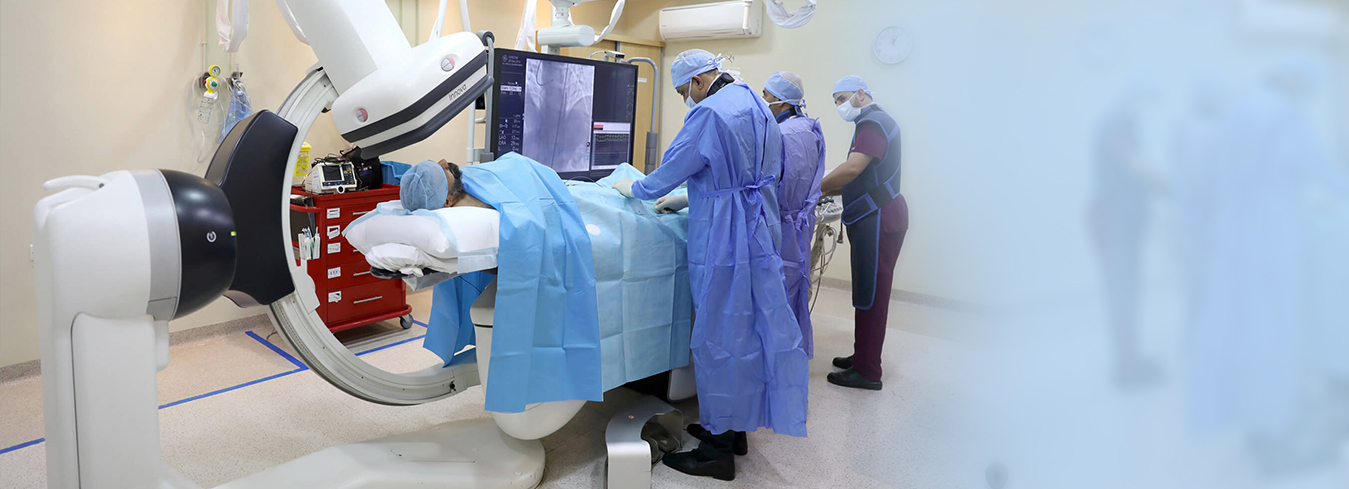
Overview
Blood cancer—also known as hematologic cancer—is a serious yet increasingly manageable condition that affects the blood, bone marrow, and lymphatic system. The most prevalent forms include leukemia, lymphoma, and multiple myeloma.
Thanks to significant advancements in oncology, particularly in India, survival rates are improving. The country has become a trusted destination for cutting-edge treatment at highly affordable prices—providing integrated services from diagnosis to post-treatment care at top-tier hospitals.
Types of Blood Cancer Treated in India
Understanding the specific type of blood cancer is crucial for determining the most effective treatment. The three main types are:
1. Leukemia
- Originates in the bone marrow and results in the abnormal production of white blood cells.
- Can be acute (fast-growing) or chronic (slow-progressing).
2. Lymphoma
- Affects the lymphatic system.
- Subdivided into:
- Hodgkin’s Lymphoma (HL)
- Non-Hodgkin’s Lymphoma (NHL)
3. Multiple Myeloma
- A cancer of plasma cells in the bone marrow.
Leads to bone degradation and weakens the immune system.
Treatment Options for Blood Cancer in India
1. Chemotherapy
- Mainline treatment for all blood cancers
- Administered in multiple cycles orally or intravenously
2. Targeted Therapy
- Attacks cancer-specific genes or proteins
- Fewer side effects compared to traditional chemotherapy
3. Radiation Therapy
- Common for lymphomas
- Aims to destroy localized cancer cells in lymph nodes or bone marrow
4. Immunotherapy
- Strengthens the immune system to combat cancer
- Includes monoclonal antibodies and checkpoint inhibitors
5. Bone Marrow / Stem Cell Transplant
- Essential for advanced leukemia and multiple myeloma
- Two types:
- Autologous (patient’s own stem cells)
- Allogeneic (donor stem cells)
6. Supportive Therapies
- Blood transfusions
- Pain management
- Antibiotics and nutritional support
- Mental health counseling
All are equipped with modern technology, cutting-edge labs, and internationally trained specialists.
Why Choose India for Blood Cancer Treatment?
- Affordability: Up to 70% cheaper than Western countries
- World-class infrastructure: JCI and NABH-accredited hospitals
- Expert doctors: Renowned oncologists and hematologists
- Comprehensive services: From diagnosis to rehab
- Quick treatment access: No long waiting periods
- International patient care: Full support with travel, visas, accommodation, interpreters
Recovery & Follow-Up Care
Post-treatment recovery is gradual and monitored through:
- Regular blood and marrow tests
- Imaging (CT, PET) scans
- Monitoring for late side effects
- Nutritional and emotional support
- Rehabilitation plans
Patients usually require follow-ups for up to 5 years.
Conclusion
India stands out as a leader in delivering high-quality, affordable blood cancer care. With top-tier medical infrastructure, experienced professionals, and personalized treatment approaches, India offers renewed hope to patients worldwide.
Choosing the right hospital and understanding the treatment journey—including costs and options—can make a critical difference in outcomes and peace of mind.
Top Hospitals for Blood Cancer Treatment
Below are the list of the top hospitals that are known for Blood Cancer Treatment procedures:

CK Birla Hospital, Gurugram
Established in: 2017
Number of Beds: 90
Multi Specialty
Location: Gurugram

Fortis Hospital, Bangalore (Bannerghatta Road)
Established in: 2006
Number of Beds: 284
Multi Specialty
Location: Bangalore

Sir Ganga Ram Hospital, Delhi
Established in: 1954
Number of Beds: 575
Multi Specialty
Location: New Delhi

Apollo Hospital Mumbai
Established in: 1983
Number of Beds: 500
Multi Specialty
Location: Mumbai

Shalby Sanar International Hospital, Gurgaon, India
Established in: 2022
Number of Beds: 150
Multi Specialty
Location: Gurugram

Medicover Hospital HiTec City Hyderabad
Established in: 2011
Number of Beds: 250
Super Specialty
Location: Hyderabad

Care Hospitals, Banjara Hills, Hyderabad
Established in: 2000
Number of Beds: 435
Multi Specialty
Location: Hyderabad

Yatharth Super Speciality Hospital Noida
Established in: 2013
Number of Beds: 1200
Super Specialty
Location: Noida

Gleneagles BGS Hospital, Bangalore
Established in:
Multi Specialty
Location: Bangalore

Continental Hospitals Hyderabad
Established in: 2013
Number of Beds: 750
Super Specialty
Location: Hyderabad
Our Services
Transparent • Professional • Without Hassles
Compare Cost Estimates
Get detailed cost breakdowns and compare prices across multiple hospitals
Book Doctor Appointment
Schedule appointments with top specialists at your convenience
Hospitalisation Support
Complete assistance from admission to discharge with dedicated care
Video Consultation
Consult doctors online or in-person based on your preference
Travel Assistance
Visa support, flight booking, and airport pickup services
Language Interpreter
Multilingual support to ensure clear communication
Accommodation
Comfortable stay arrangements near the hospital
24/7 Support
Round-the-clock assistance for all your medical needs
Top Blood Cancer Treatment Specialists

Dr. Amit Agarwal
Delhi4.0
Experience: 32+
Education: Director , MBBS, MD, DM
Get a free consultancy

Dr. Harit Chaturvedi
Delhi4.0
Experience: 38
Education: MBBS , MS, MCh
Get a free consultancy

Dr. Dharma Choudhary
Gurugram4.0
Experience: 28
Education: MBBS, MD , DM, Fellowship
Get a free consultancy

Dr. Puneet Gupta
Faridabad, India4.0
Experience: 28
Education: MBBS, MD, DNB, DM, MBA
Get a free consultancy

Dr. Mohit Agarwal
Delhi4.0
Experience: 20
Education: MD, DNB, ECMO (EUROPE), PDCR, MRCP
Get a free consultancy

Dr. Ashish Goel
Noida4.0
Experience: 32
Education: MBBS , MS , DNB , MNAMS
Get a free consultancy

Dr. Praveen Bansal
Faridabad, India4.0
Experience: 25
Education: MBBS , MD , DM
Get a free consultancy

Dr. Anshuman Kumar
Delhi4.0
Experience: 25+
Education: MBBS, MS, MCh, MRCS
Get a free consultancy

Dr. Vedant Kabra
Gurgaon4.0
Experience: 29
Education: MBBS, MS. DNB MRCS(Edin), MNAMS, FIAGES
Get a free consultancy

Dr. Rajasundaram
Chennai, India4.0
Experience: 32
Education: MBBS, MS, MCh, DNB, FAIS, FAMS
Get a free consultancy
Get Free Consultation
Fill out the form below and our team will get back to you shortly
Symptoms
Common Symptoms of Blood Cancer
- Persistent fatigue
- Frequent or severe infections
- Sudden weight loss
- Unusual bruising or bleeding
- Swollen lymph nodes
- Bone or joint pain
- Fever, chills, or night sweats
Before the Procedure
Pre-Procedure
Before starting cancer treatment, the primary concern is to analyze the cancer stage. The diagnosis of blood cancer involves several key steps. It begins with a thorough medical history and physical examination, where the doctor gathers information about symptoms and checks for signs such as swollen lymph nodes. A complete blood count (CBC) is performed to analyze blood levels, including red and white blood cells, hemoglobin, and platelets, helping to identify abnormalities indicative of blood cancer. A peripheral blood smear is then conducted to examine blood samples under a microscope for abnormal cell shapes and sizes. If necessary, a bone marrow biopsy is performed to collect a sample from the hip to assess for cancerous cells. Flow cytometry may be used to analyze blood or bone marrow samples to differentiate between normal and cancerous cells. Genetic testing is conducted to identify any mutations or abnormalities, which can inform prognosis and treatment. Imaging tests, such as X-rays, CT scans, or MRIs, are also utilized to evaluate the extent of the disease and check for tumors. In some cases, a lymph node biopsy may be required if lymph nodes appear swollen. Finally, all test results are compiled to provide a definitive diagnosis, which will guide the treatment plan.
Blood cancer is determined as stages based on the level of metastasis. Metastasis is nothing but the deposition of abnormal cancer cells elsewhere in the body apart from its origin. According to the symptoms and the pace of metastasis, the various stages of blood cancer are differentiated.
Stage 1: The primary stage incorporates an increase in the lymph node size. This occurs because of the sudden abnormal multiplication of the lymphocytes. The prognosis of this stage is good considering there is no involvement of other parts of the body.
Stage 2: In the subsequent stage, the lymph nodes with the spleen and liver get involved and enlarged. With the involvement of visceral organs, the abnormal growth of lymphocytes is exceptionally high at this stage.
Stage 3: At the level of this stage, the abnormal lymphocytes hamper the production of the other blood cells like red blood cells. There is a resultant anemic condition. Also, there is a spread of metastasis to more than two organs.
Stage 4: This is the last stage of blood cancer with a high-risk proportion. The number of platelets in the blood begins to drop rapidly. The impacted cells begin harming the lungs and different organs. The organs affected earlier get severely affected.
During the Procedure
What are the treatment options available for Blood cancer?
Stem Cell Transplantation
Stem cell transplantation is a crucial medical procedure that involves replacing diseased bone marrow with healthy bone marrow. This treatment typically requires high doses of chemotherapy or high-frequency radiation to eliminate existing cancer cells, which may be present in the bone marrow or lymph nodes. The healthy blood-forming hematopoietic stem cells are then injected through a venous puncture, enabling the production of normal and healthy blood cells necessary for the body’s proper functioning.
Stem cells can be derived from various sources, leading to different types of transplant procedures:
- Bone Marrow Transplant (BMT): Stem cells are harvested from the bone marrow.
- Peripheral Blood Stem Cell Transplant: Stem cells are collected from the bloodstream.
- Cord Blood Transplant: Stem cells are sourced from the blood of the umbilical cord.
There are two primary types of stem cell transplantation based on the donor:
- Autologous Transplantation: The stem cells come from the patient’s own body, allowing for a personalized treatment approach.
- Allogeneic Transplantation: The stem cells are obtained from a donor, which can be a family member or an anonymous donor.
The primary goal of stem cell transplantation is to replace cancerous cells with healthy ones, leading to a reduction in symptoms and an overall improvement in the patient’s quality of life.
Chemotherapy
Chemotherapy is one of the main treatments for blood cancer, employing various chemical agents to target and destroy cancer cells. This treatment is generally considered a milder form of therapy compared to more aggressive approaches, resulting in fewer side effects.
The process involves using specially designed chemicals that not only eliminate abnormal cancer cells but also inhibit their ability to multiply. Depending on the specific condition and severity of the disease, patients may receive either a single type of drug or a combination. These medications can be administered in pill form or through intravenous injections directly into the bloodstream.
Radiation Therapy
Radiation therapy is another important treatment modality used to combat cancer. It employs high-intensity radiation to kill cancer cells and prevent their overgrowth. During this procedure, patients lie on a treatment table while a large radiation machine rotates around them, focusing beams of radiation on specific areas affected by cancer.
This type of therapy is often recommended before undergoing stem cell transplantation to reduce the overall cancer burden in the body.
Targeted Therapy
Targeted therapy is designed to specifically target and destroy malignant blood cells without harming normal cells. This therapy focuses on proteins present in cancer cells to halt their growth and promote apoptosis, or programmed cell death.
Two common types of targeted therapies include:
- Monoclonal Antibodies: These agents specifically bind to cancer cells, blocking their function and aiding the immune system in identifying and attacking them.
- Small Molecule Drugs: These drugs interfere with the proliferation of cancer cells. For example, angiogenesis inhibitors prevent the formation of new blood vessels that supply nutrients to tumors, effectively starving them and causing them to shrink.
Immunotherapy
Immunotherapy harnesses the body’s immune system to identify and destroy cancer cells. This treatment can significantly slow the growth of cancer cells or eliminate them altogether. Immunotherapy sessions typically last from one week to several weeks and are usually administered through intravenous injections.
While immunotherapy is generally well-tolerated, some patients may experience side effects, which can vary based on the specific agent used. Common side effects include rashes, swelling at the injection site, headaches, muscle aches, fever, and general fatigue.
Types of immunotherapy include:
- Cytokines: These are proteins produced by white blood cells that help regulate immune responses and slow cancer growth.
- Gene Therapy: This involves introducing genetic material into cancer cells using a viral vector to induce their destruction.
Monoclonal Antibodies: Laboratory-produced antibodies that assist the immune system in recognizing and attacking cancer cells.
After the Procedure
Post Procedure
The primary aim of most blood cancer therapies is to alleviate symptoms and reduce the growth of cancer cells. Once treatment is completed, healthcare providers conduct follow-up tests similar to those performed during diagnosis to check for any remaining cancer cells in the body.
Based on these follow-up results, additional treatment options may be recommended, tailored to the patient’s specific health status and needs.
Risks & Complications
What are the Risks & complications associated with blood cancer treatment?
The risks and complications regarding blood cancer treatment vary from person to person. Each of the cases may respond to the respective treatment differently. This may involve short term side effects and long term side effects
- Short-term side effects are experienced by the patient during the treatment or shortly after it.
- Long-term side effects may start slowly and could last for a long time. These side effects could be for a month or a year. Sometimes it may even take several years to wean off.
Treatment Costs in India
Blood Cancer Treatment Cost in India
Costs vary depending on the type and severity of cancer, city, hospital, and treatment duration.
| Treatment Component | Cost (INR) | Cost (USD) |
| Diagnostic Tests & Biopsy | ₹30,000 – ₹70,000 | $360 – $840 |
| Chemotherapy (per cycle) | ₹25,000 – ₹1,50,000 | $300 – $1,800 |
| Chemotherapy (6–8 cycles total) | ₹1,50,000 – ₹10,00,000 | $1,800 – $12,000 |
| Targeted Therapy (monthly) | ₹75,000 – ₹2,50,000 | $900 – $3,000 |
| Bone Marrow Transplant | ₹10,00,000 – ₹25,00,000 | $12,000 – $30,000 |
| Radiation Therapy (if needed) | ₹1,00,000 – ₹3,00,000 | $1,200 – $3,600 |
| Hospital Stay & ICU Charges | ₹1,00,000 – ₹2,50,000 | $1,200 – $3,000 |
| Medications & Supportive Care | ₹50,000 – ₹2,00,000 | $600 – $2,400 |
Factors Affecting the Cost of Treatment
- Cancer type and stage
- Hospital location (Tier-1 vs Tier-2 cities)
- Treatment complexity (e.g., bone marrow transplant, CAR-T therapy)
- Length of hospital stay
- Type of bone marrow transplant (autologous vs allogeneic)
International vs Indian patients (visa, accommodation, and administrative expenses)
Frequently Asked Questions
Frequently Asked Questions (FAQs)
- What types of blood cancer are treated in India?
Leukemia (acute/chronic), Lymphoma (Hodgkin’s & Non-Hodgkin’s), and Multiple Myeloma—all with personalized treatment plans. - What’s the average cost of blood cancer treatment in India?
₹5,00,000 to ₹25,00,000 ($6,000–$30,000), depending on treatment type and hospital. - Why do international patients choose India?
India offers cutting-edge technology, skilled specialists, English-speaking support, and much lower treatment costs. - What are the main treatment options?
Chemotherapy, radiation, targeted therapy, immunotherapy, bone marrow transplant, and supportive care. - How long does treatment take?
Chemotherapy spans 3–6 months. Bone marrow transplants require several weeks in hospital and months of recovery. - How much does a bone marrow transplant cost?
₹10–25 lakh ($12,000–$30,000), depending on transplant type. - Is financial assistance available?
Yes—through government schemes, CSR programs, NGOs, and insurance plans (terms vary). - Which hospitals are considered the best?
Tata Memorial, Apollo, Fortis, BLK-Max, CMC Vellore, and Rajiv Gandhi Cancer Institute. - Is donor matching for transplants available in India?
Yes—HLA matching is widely available, with access to national and global donor registries. - What is the success rate?
Leukemia: up to 90% in children
Lymphoma: 70–85% with early treatment
Multiple Myeloma: Improved survival due to new drugs
Top hospitals in India match global success benchmarks.
11. Do Indian hospitals support international patients?
Absolutely—services include visa help, airport pickup, interpreters, accommodation coordination, and transparent billing.